On Thursday 12 March, everyday life remained relatively normal across the UK. The back pages of the newspapers were dominated by the victory of Atletico Madrid over Liverpool – 50,000 fans had crammed into Anfield stadium.
Throughout that day shoppers shopped, while millions drove to work or poured out of trains into city centres.
And in the evening, people went out.
At Wembley Arena, Lewis Capaldi sang to an audience of 12,000 fans – having urged them to bring hand sanitiser with them. Around the UK people headed for events big and small.
But these were not normal times. A new coronavirus was spreading across the globe.
On that day, Italy was shutting all non-essential shops and the Republic of Ireland announced that schools would close.
But looking back, the question that will always be asked is – did the UK go into lockdown too slowly? Should those crowds have been out that day?
The World Health Organization (WHO) had been asking countries to do everything they could to contain the infection since late February.
And some countries were scaling up test and trace to try to suppress the virus.
But on 12 March, the UK had all but abandoned community testing to focus on those sick enough to be admitted to hospital. At the time, there were 590 known cases of coronavirus in the UK – more than four times the number in the previous week.
The government announced it was moving out of the “contain” phase into the “delay” phase. The risk level was raised to high, and anyone with symptoms was asked to self-isolate for a week.
The lockdown was yet to start.

At a press conference Prime Minister Boris Johnson, his chief scientific adviser Sir Patrick Vallance and chief medical officer Prof Chris Whitty explained the policy to keep schools open and to allow major public events to go ahead.
Johnson said that according to scientific advice, banning major public events would have little effect on the spread of the disease.
Prof Whitty argued that beginning social distancing measures “too early” would risk people becoming tired of them and public compliance waning.
And Sir Patrick began to talk about the concept of herd immunity. Speaking about the coronavirus he said: “It’s not possible to stop everybody getting it and it’s also actually not desirable because you want some immunity in the population. We need immunity to protect ourselves from this in the future.”
Mr Johnson reiterated that people should remember to wash their hands.
The next day tens of thousands of people poured into Cheltenham Racecourse to watch the Gold Cup.

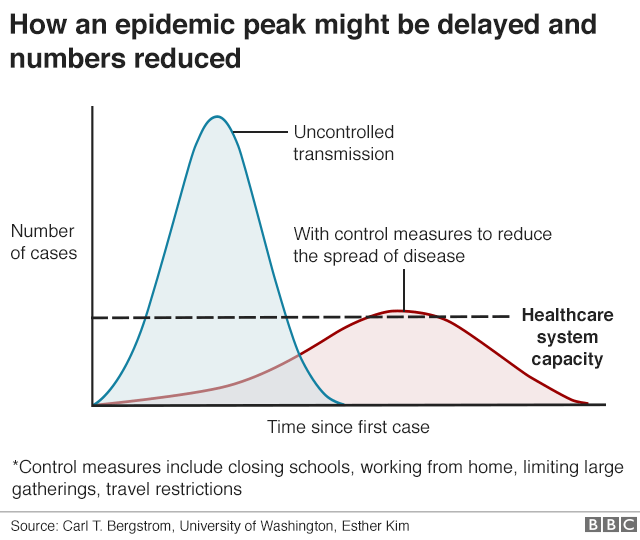
Sir Patrick was on BBC Radio 4’s Today programme. He said the thinking behind the government’s approach was to try to “reduce the peak”, and because most people would only get a “mild illness”, to “build up some degree of herd immunity… so that more people are immune to this disease and we reduce the transmission”.
At the same time, he said, the vulnerable would need to be protected from the virus.
In response to a question asking whether it would be a “good thing” to allow the disease to spread widely now, rather than later, Sir Patrick replied he didn’t want high numbers of infections over a short period of time, overwhelming the NHS.
“So that’s the flattening of the peak. You can’t stop it, so that you should end up with a broader peak, during which time you would anticipate that more people will get immunity to this and that in itself then becomes a protective part of this process.”
He said previous epidemics had shown that measures to strongly suppress the virus risked it bouncing back when they were ended.
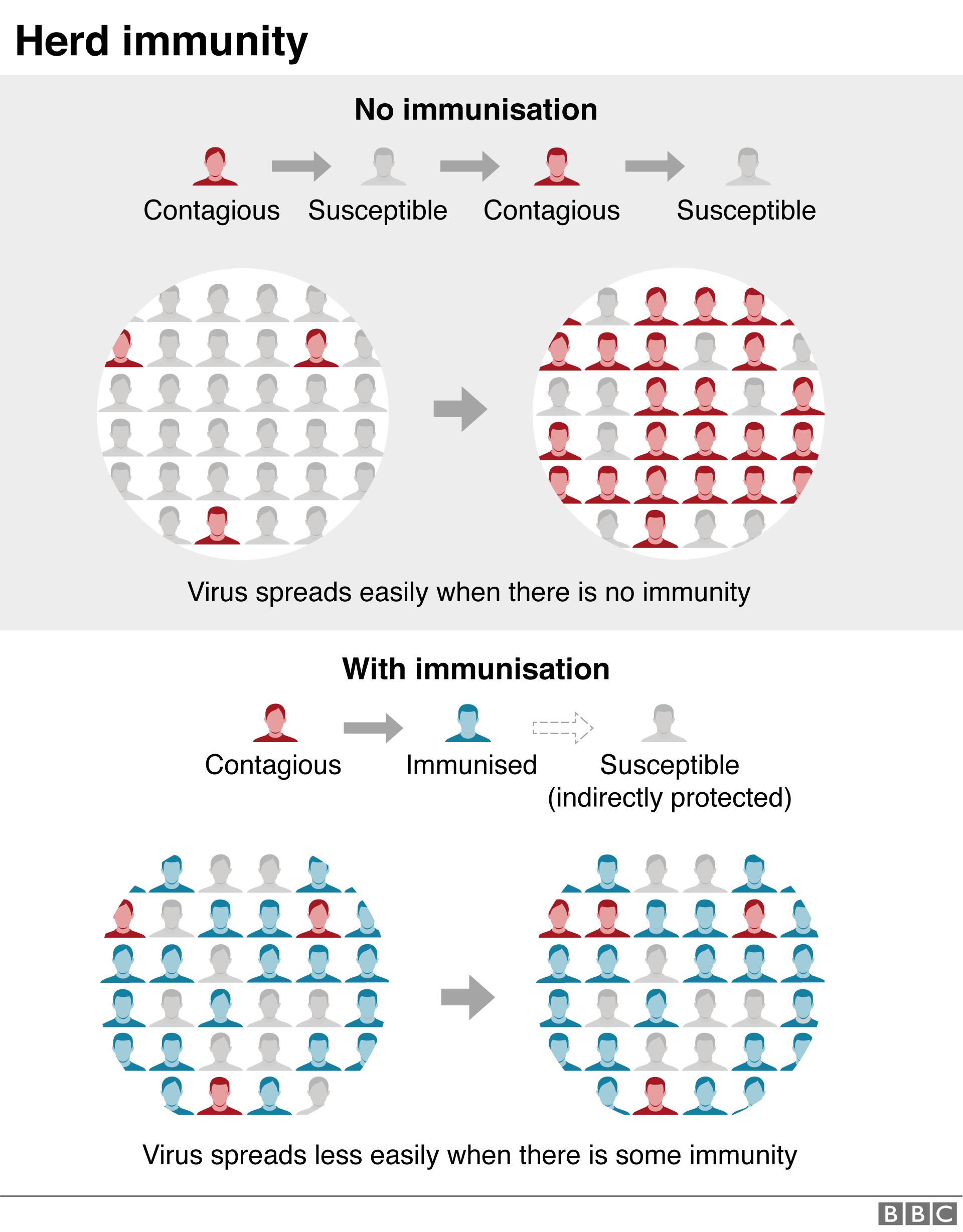
Herd immunity
“Herd immunity” is a concept describing the point at which a population has developed protection against a disease.
There are two ways to do this. Vaccination is one route. But with any new virus it’s impossible to say how long it will take to develop a vaccine, if ever.
The other way is for people to catch the disease and build up some form of immunity. If exposed to the virus again, it is assumed they have protection. If most people in a population are protected then the virus cannot spread.
But there are two problems. One is that with a new virus – like this particular coronavirus – it’s not always clear how much protection having had the disease, particularly a mild case, gives you or how long it lasts.
And if most of the population catches the disease, many thousands might die.
On 13 March, Sir Patrick stated that about 60% of the population would need to become infected for society to have “herd immunity” – effectively some 40 million people in the UK.
“Communities will become immune to it and that’s going to be an important part of controlling this longer term,” he told Sky News.
These comments sparked an immediate backlash.
Anthony Costello, professor of health and sustainable development at University College London and a former director of maternal and child health at the WHO, tweeted: “Is it ethical to adopt a policy that threatens immediate casualties on the basis of an uncertain future benefit?”
And Dr Margaret Harris from the WHO told the BBC’s Today programme on 14 March: “We don’t know enough about the science of this virus. We can talk theories, but at the moment we are really facing a situation where we have got to look at action.”
That day, more than 200 scientists – ranging from experts in mathematics to genetics – signed an open letter to the government urging it to introduce tougher measures to tackle the spread of Covid-19.
“We consider the social distancing measures taken as of today as insufficient, and we believe that additional and more restrictive measures should be taken immediately.”


‘Heart of the health service’
The government tried to play down the words that had sparked the furore.
A spokesman for the Department of Health and Social Care said Sir Patrick’s comments had been misinterpreted. “Herd immunity is not part of our action plan but is a natural by-product of an epidemic,” he said.
That same evening, the Telegraph website published an article by the Health Secretary Matt Hancock.
“We have a plan, based on the expertise of world-leading scientists. Herd immunity is not a part of it. That is a scientific concept, not a goal or a strategy.”
On Sunday 15 March, the health secretary appeared on the BBC’s Andrew Marr and Sky’s Sophy Ridge programmes, restating that herd immunity was not the government’s policy.

The Telegraph website said the government had appeared to “U-turn on the idea”. The Express said herd immunity had been abandoned after “a huge backlash”.
But despite repeated government denials, the BBC has learned that on 13 March, when Sir Patrick Vallance was outlining the government’s approach to tackling the virus, herd immunity was being discussed at the heart of the health service.
From the start of the outbreak, Simon Enright, director for communications for NHS England and NHS Improvement, would offer weekly briefings to media teams in other health organisations and medical royal colleges. He and his team would share some of the latest information on strategy and thinking.
The BBC has seen contemporaneous notes from the meetings and spoken to people on the calls.
At the meeting on 13 March, Mr Enright is said to have relayed information from the government’s top scientific and medical advisers.
The notes say the communications chief shared NHS England’s own advice on holding internal work events, but say “we are not telling you what to do”.
“We want people to be infected with Covid-19,” the notes say. “The best way of managing it is herd immunity and protect the vulnerable.”
Mr Enright was clear where the idea had come from, according to the notes. It was on the “direct advice” of the chief medical adviser and chief scientific adviser.
NHS England had cancelled one of its own events but only so staff could be retained to work on the coronavirus response, according to the notes.
“In other words – if you cancel events to stop people coming out of service that’s fine, but don’t cancel because of risk of infection.”
NHS England says Mr Enright was paraphrasing what he had heard Vallance say on the Today programme that morning, and other comments made in the press briefings and interviews.
“This is chaos,” says Richard Horton, editor of the medical journal The Lancet, who has criticised what he sees as the failure to heed early warnings from China. “This is no way to manage a pandemic.
“What it shows is that at the heart of the government’s response there was no clear command-and-control structure as to how we were going to manage this outbreak.
“It’s very important to get these facts on the record about herd immunity, because history is being rewritten at the moment and herd immunity is being written out of the history.”
A government spokesperson said: “This is a new virus and an unprecedented global pandemic, and our strategy to protect, delay, contain, research and mitigate was clear from the outset. It is categorically wrong to suggest herd immunity was the government’s aim.”


Suppression versus mitigation
Some critics believe it is problematic if herd immunity was part of the government’s thinking at the time.
Sir David King, former chief scientific adviser to the government between 2000 and 2007, has been a vocal critic of the UK government’s efforts to fight coronavirus.
“I can only give you one rational explanation for this tragedy and that is that they had decided to go for herd immunity. We did hear the phrase ‘herd immunity’, although the government subsequently somehow denied that they were doing that.”
There are plenty of experts who now believe an earlier lockdown would have saved lives.
Prof Neil Ferguson, an epidemiologist and former government adviser, told a committee of MPs on 10 June the number of coronavirus deaths could have been halved if lockdown had been introduced only a week earlier.

But the prime minister responded to Prof Ferguson’s comments hours later at the No 10 press conference that day, saying it was “simply too early to judge ourselves”.
“We made the decisions at the time on the guidance of Sage [the government’s scientific advisory group], including Prof Ferguson, that we thought were right for this country,” he said.
The BBC has spent months speaking to more than a dozen scientists advising the government on its response to the outbreak to try to find out just how important the concept of herd immunity was to the scientific thinking that drove government strategy at the beginning of the outbreak.
Some of Sage’s papers model different ways of responding to the outbreak.
Two of the options when responding to a disease like Covid-19 are known as suppression and mitigation, according to Dr Thomas House, a statistician from the University of Manchester and a member of the modelling group (SPI-M) that feeds into Sage.
Suppression, he says, aims to reduce infections to zero, while mitigation accepts the inevitability of an outbreak and concentrates efforts on minimising suffering.
“If a tsunami is coming we don’t try to stop the tsunami, we just try to ensure that the minimum number of people are harmed by it.”
“Herd immunity was on the table,” says Prof Ian Hall, an epidemiologist, head of the University of Manchester modelling team, and a member SPI-M who has also attended multiple Sage meetings.
He described it “as a concept”, a technical term typically used when discussing the spread of disease.
Dr Hall says SPI-M discussed a range of options to be able to prevent the NHS being overwhelmed and buy it time to prepare, while the population achieved “some sort of herd immunity”.
Herd immunity can be achieved by an uncontrolled spread of infection which can happen quickly, but that would overwhelm the NHS. Hall says this was never realistic because the government would always act to reduce the number of deaths.
But it can also be achieved by measures to mitigate the disease which look to protect lives, in the absence of any vaccine, and build up immunity over a long time.
Jeremy Hunt, chairman of the health and social care select committee, has criticised the scientific advice at the start of the pandemic, calling it “wrong”.
“Ministers were given the choice of extreme lockdown or mitigated herd immunity,” he recently told the Times newspaper.
He said that Sage did not model the adoption of a testing regime used in previous coronavirus outbreaks in East Asia.
“We were unfortunately following a flu policy, not Sars (Severe Acute Respiratory Syndrome).”


Flu pandemic
The government has spent much of the past decade preparing for a flu pandemic – something consistently rated the number one natural hazard threat on the National Risk Register of Civil Emergencies.
Devi Sridhar, professor and chairwoman of global public health at University of Edinburgh’s Medical School, says the 2011 flu plan – which still forms the basis of a planned response to such a pandemic – appears primarily concerned with mitigating the impact of the virus.
“This was very much the view that you could not control or contain this outbreak,” she says. “[The virus is] going to run through, it’s inevitable, it’s unstoppable.”
Sridhar, who is also a member of the Scottish government’s Covid-19 advisory group, says the initial UK response looked like it was “largely out of the ‘flu playbook'”.
“It was the idea that you don’t want to disrupt people’s lives. You want to keep things moving but you have to mitigate or take care of the health consequences as it flows through.”


Lockdown
Dr Hall remembers the moment he began to question how close the UK was to emulating scenes in Italy.
He and a team at the University of Manchester had spent weeks hunched over laptops modelling how the disease might spread in the UK.
In mid-March, he was approached by some Chinese students at the university demanding to know why the UK was not acting faster, in line with the Chinese government’s response.
Dr Hall told them that scientists were not sure that transmission of the disease would be similar in the UK because of differences between the two countries.
But the students’ questioning got him and the team thinking.
Scientists had agreed the amount of time it was taking for infections to double was between five and six days, in a Sage consensus statement on 16 March.
But the Manchester team were concerned it could be much shorter, and the virus was spreading more rapidly.
After days of scrutinising data, Hall and the team found that the total number of positive swabs in Italy and the UK were doubling much faster, closer to every three days. They presented this to SPI-M on 20 March.
The NHS was now just 14 days from being overwhelmed, according to their projections.
It took another three days for SPI-M modelling groups across the country, working with different data, to agree.
In the meantime, infections were rising exponentially, meaning every day was critical.
On 16 March, a crucial report was published by a team from Imperial College led by Prof Ferguson.
It looked at three scenarios:
- doing nothing and letting the virus spread
- a mitigated approach where the spread of the disease was accepted but measures were taken to slow it
- Suppression, effectively trying to stop the epidemic in its tracks, and bringing cases down as low as possible

In the first scenario the modelling projected 500,000 dead, but even in the mitigated approach potential deaths were estimated at 250,000 with the NHS being completely overwhelmed.
Over the next seven days after the release of the report, an escalating series of actions was taken. On 16 March the government set out its social distancing policy, on 18 March it announced schools would be closed and on 20 March pubs, bars, cafes, restaurants, clubs, theatres, cinemas and gyms were all closed with immediate effect.
Then on 23 March full lockdown was announced in an address to the nation by Boris Johnson. Non-essential shops were closed and people were ordered to stay home.

And yet Prof Ferguson says he had already provided the government by early March with estimations of the likely number of deaths if a mitigation strategy was pursued – at least 305,000. This was revised down to 250,000 in the report he published on the 16 March but the NHS would still be over capacity.
“Our projections of the potential health impact of the pandemic were known from about 5 March onwards,” he says. They were “actively discussed” within government, he adds.
Prof Ferguson says he told Sage the findings were his best estimate of what was most likely to happen.
He says other scientists had reached similar conclusions too.
But Sage only considered these a reasonable worst-case scenario – of the kind used by the government to plan for a range of eventualities – and not a forecast of what was most likely to happen.

There were other early voices providing key pieces of information in that time.
The BBC has been told that NHS England’s medical director Stephen Powis informed Sage as early as 13 March that projections predicted the NHS would not have capacity to cope under a strategy which looked only to mitigate the spread of the virus and not suppress it.
“If that result was known on 5 March that’s devastating,” says Richard Horton. “We wasted over two weeks when the virus was exponentially growing through communities up and down the country.”
“This information should have been publicly available to be scrutinised by other experts so that we could have had a public discussion and built public support for an early lockdown.”


Protecting the vulnerable
Scenes of hospitals being overwhelmed, such as those in northern Italy, were never replicated in the UK.
But in March, the virus was spreading inside care homes.

The need to “protect the vulnerable” had been mentioned repeatedly by the government and its advisers.
Graham Medley, chairman of SPI-M, gave an illustration of the challenges of delivering this when explaining herd immunity on BBC’s Newsnight on 12 March.
He argued that theoretically – although impractically – one way to achieve it would be to move all vulnerable people to the north of Scotland, and the rest of the population to Kent.
That way “a nice big epidemic” in Kent would allow herd immunity and the re-mixing of the entire country again, he said.
“We can’t do that, so what we’re going to have to try and do, ideally, is manage this acquisition of herd immunity and minimise this exposure of people who are vulnerable.”
Dr Hall, co-chair of the Sage group advising on care homes, told the BBC that forecasts of the spread of infections in care homes were not conducted until early April. It was not done previously because of a lack of data on the outbreak in care homes.
“We didn’t see the care home outbreaks back in March arising,” he says.
Dr Hall says the links and infection risk between care homes, hospitals and the community were not well documented.
“I didn’t appreciate personally the level of the amount of staff that move between care homes and the potential for staff to introduce disease,” he says.
Health Secretary Matt Hancock has on many occasions defended the government’s handling of the outbreak in care homes, insisting that from the beginning it had tried to throw a “protective ring” around them.


Questions
Four months on from the introduction of the lockdown, scientists remain unsure how long any immunity from coronavirus might last.
No-one knows when an effective vaccine will come.
But Dr Hall says the UK’s response will ultimately end with herd immunity.
“Without a vaccine we will go on with transmissions at a relatively low level hopefully and with contact tracing and all the other interventions to mitigate the disease, we will eventually achieve herd immunity one way or another.”
But that could take years.

For Prof Ferguson, the issue with the suppression strategy is it leaves many countries without a long-term exit plan and “stuck in the same policy” until a vaccine is found.
The fear is that as soon as restrictions are lifted, the virus will return across borders.
Only very few countries, such as New Zealand and Taiwan, have come close to eliminating the virus, he said.
Questions about the timing of policy decisions and the scientific advice that guided the response may take some time to answer. The prime minister recently committed to an inquiry, but no timeframe has been given.
Sir Patrick told a Commons science committee on 16 July that it was “clear that the outcome has not been good in the UK”. He said that there were many factors to be considered when determining how a country has responded to the outbreak.
“There will be decisions made that will turn out not to have been the right decisions at the time,” he said.
Sir David King says that, “When it comes to the inquiry, the politicians will say, ‘We were just following the scientific advice.'”
But King, like many of the scientists we spoke to, complains that this suggests there is one definitive view. These scientists point out that there are differing views and the government’s actions are ultimately based on political decisions.
The Prime Minister, Boris Johnson, Health Secretary Matt Hancock, chief medical adviser Prof Chris Whitty and chief scientific adviser Sir Patrick Vallance declined to give an interview.
A government spokesperson told the BBC: “At every stage, we have been guided by the advice of experts from Sage and its subcommittees, and our response ensured the NHS was not overwhelmed even at the virus’ peak, so that everyone was always able to get the best possible care.”
But for the critics the danger is a second wave of infections will come without lessons having been learnt from the first.
Credit: Source link